
In this post I discuss the benefits of functional medicine for fatigue and CFS/ME, explain the role of mitochondria in energy availability and outline 20 causes of fatigue. I will end with a brief outline of some of the tools and lab tests I use to put functional medicine, naturopathy and nutritional therapy principles into practice at my fatigue and CFS/ME clinic in London, Devon and online.
Natural fatigue and unhealthy fatigue
Fatigue is natural in response to physical or mental exertion or simply staying awake for too long. Throughout this post when I use the word ‘fatigue’ I am referring to fatigue that is extended in duration, or that arises disproportionately to the exertion and doesn’t resolve with rest as it should do in a healthy body.
Why work with functional medicine for fatigue & CFS/ME?
CFS/ME severely impacts quality of life
It is only when we lose our capacity to generate energy in a usable form that we understand how vital it is to even the simplest of tasks that most of us take for granted in our daily lives. In Chronic Fatigue Syndrome (CFS) and Myalgic Encephalomyelitis (ME) not just physical energy but mental energy is vastly diminished. The stamina to carry out the simplest of tasks is lacking such that even a phone conversation whilst lying in bed could be enough to send a CFS/ME sufferer into an energy crash which could take a few days to recover from, and by ‘recover’ here I mean coming back to the current baseline of fatigue, which may mean being bed bound most of the time.
CFS/ME sufferers are barely able to generate the energy needed just to maintain the physiology and biochemistry necessary for survival. Less than optimal biochemical shortcuts may be taken by the under-resourced body, leading to various biochemical and physiological vicious cycles and a wide array of debilitating symptoms beyond severe fatigue. These could include brain fog, insomnia, dizziness, aches and pains, muscular weakness, headaches, gut disturbances, poor temperature regulation and sensitivity to noise, light and sound.

My personal experience with CFS/ME
I have personally experienced CFS/ME for about a year which led me to research more deeply into health and nutrition, sparking an interest that led to my current clinical work as a functional medicine practitioner, nutritional therapist and naturopath.
At the time my brain speed was so slow that I would not remember what I was going to get whenever I was opening a drawer or cupboard in my kitchen, so that preparing a meal took far longer than it otherwise would, perhaps 2 to 3 times as long!
There is so much mental processing we take for granted even in cooking a simple meal, listening to music or watching a film that might otherwise give us pleasure, and it all requires energy!
I remember having to walk uphill very slowly (learning not to try to compete with people twice my age) and once I even forgot to take £50 out of the cash machine (which someone walked off with by the time I realised I had no cash to pay for my food in the shop just around the corner).
I would describe this kind of life, in which the simplest of mental and physical tasks become overwhelming, as ‘old age come early’, and yet I consider my case of CFS/ME to have been very mild.
How fatigue that is not CFS/ME also severely impacts quality of life
Both mental and physical fatigue can severely impact your quality of life. Even if you do not have the delayed fatigue that is a hallmark of CFS/ME you may lack the energy to engage with your children, to work effectively and to enjoy social events and activities that you once enjoyed. This can all add to your burden of stress and negatively impact your mood and general wellbeing.
Functional medicine investigates the root causes of fatigue and CFS/ME
Fatigue may gradually creep up on us over the years and we may assume it is ‘just’ ageing, but there are many potential mechanisms that could be causing your fatigue that can be impacted by appropriate dietary and lifestyle changes.
In the case of fatigue with a more sudden onset and of more severity these mechanisms, or root causes, may be more entrenched and vicious cycles of fatigue may have developed, but the root causes can also be worked with.
One of the fundamental principles of functional medicine is to investigate root causes of disease so as to find the most effective evidence-based dietary and lifestyle changes for you as an individual.
By focusing on dietary and lifestyle interventions, the functional medicine approach can reduce dependence on medications with their potential side-effects.
Before I discuss some of the root causes of fatigue it will be helpful to understand something about how energy in a form that our body can use is generated inside your cells.
Mitochondria – the bacteria that power us
What are mitochondria?
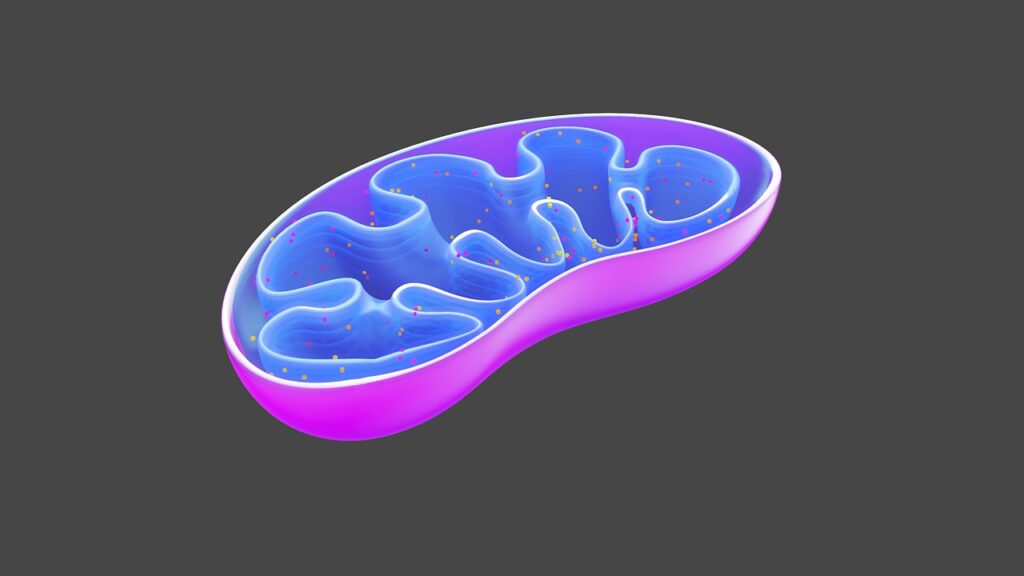
Mitochondria are organelles with a very interesting history. (You could think of organelles as the functional subunits of a cell).
Mitochondria perform many functions, but what they are best known for and what I will focus on here is their role in generating molecules such as ATP which can readily be used by the cells of your body as a source of energy.
Mitochondria are found in every cell of your body except for red blood cells.
Do mitochondria make energy?
It is a fundamental law of physics that energy cannot be created or destroyed, it can only change its form. So when you hear of mitochondria being generators of energy that is not correct.
The mitochondria change the energy held in chemical bonds from molecules derived from food into energy held in chemical bonds in molecules such as ATP (adenosine triphosphate). Then perhaps your muscles will use up this ATP by cleaving part of the molecule (a phosphate group) off to form a new molecule (adenosine diphosphate or ADP) and the chemical energy released from that chemical bond might be converted into the kinetic energy of a football you have kicked that is now flying into goal, for example.
So mitochondria do not generate energy per se, but they do generate what I will call ATP energy.
The fascinating origins of mitochondria
According to the most prevalent and most accepted (though not fully settled) theory the fascinating history of mitochondria is as follows.
A couple of billion years or so ago, algae began to generate oxygen as a byproduct of photosynthesis. When the atmosphere became rich in oxygen it posed a challenge for life on earth because oxygen is damaging to cells, causing oxidation.
Luckily for us multicellular beings a bacteria evolved that could use oxygen to generate a large amount of ATP energy from fuels like glucose. Even luckier for us this bacteria ended up inside cells and generating ATP energy for these cells.
The average cell of a multicellular organism has vastly greater energy requirements for the growth, maintenance and survival of each cell when compared to the one cell of a unicellular organism. The evolutionary leap from unicellular to multicellular life couldn’t have happened without these bacteria.
These bacteria are what we now call our mitochondria, and they retain their own DNA.
We inherit out mitochondria from our mothers, so if you have fatigue don’t blame Dad!
Are mitochondria bacteria?
So when did these bacteria become mitochondria? Are they actually bacteria, bacteria that power us and upon which we are completely dependent? This is a question that some are considering (1) and perhaps the question really is of how we define bacterium and mitochondrion.
It’s also interesting to consider what are we, or what are our bodies? What is human and what is bacterial? If all of our cells except for red blood cells depend on bacteria and our gut microbiome is made up of bacteria., fungi and viruses then what does it mean to be a human when there is so much we are completely dependent on that has microbial DNA?
Antibiotics target mitochondria because they are akin to bacteria
Whether or not you think of mitochondria as bacteria, they certainly bear a lot of structural similarity to bacteria and for this reason may be targeted by antibiotics. Fluoroquinolone antibiotics in particular are a class of antibiotics known to damage mitochondria and can cause debilitating fatigue, muscle weakness, cognitive dysfunction and dysautonomia in some individuals (2, 3).
What is dysautonomia?
Your autonomic (involuntary) nervous system regulates functions such as blood pressure, heart rate and body temperature and fluoroquinolones can cause symptoms of the condition known as dysautonomia, which you could understand as a failure of the autonomic nervous system. Symptoms of dysautonomia could include very low blood pressure, faintness and dizziness, poor temperature regulation and rapid heartbeat.
Fluoroquinolone antibiotics causing dysautonomia demonstrates how essential mitochondria are
Neurons have a high demand for ATP energy and are thus particularly rich in mitochondria, which means they could be particularly prone to failure when targeted by fluoroquinolone antibiotics, thus causing dysautonomia (4, 5).
I hope this example of mitochondrial dysfunction helps you to appreciate how essential the health of your mitochondria are for you to perform even the most basic and unconsciously controlled functions that we normally take for granted.
How we produce ATP energy inside and outside the mitochondria – glycolysis and oxidative phosphorylation
One of the functions of mitochondria is to generate energy in a usable form (mostly as ATP) and here I will give a brief outline of how this happens and why the ATP energy produced by mitochondria is so essential for overall usable energy production.
Glycolysis
Consider a glucose molecule in one of your cells to be oxidised so that you can make use of its energy.
Your glucose molecule can first generate some ATP outside of the mitochondria in a process known as glycolysis, which also generates a molecule of pyruvate. This will generate 2 molecules of ATP and also some energy in the form of 2 molecules of NADH.
Oxidative phosphorylation
The pyruvate molecule can then cross a mitochondrial membrane and once inside the mitochondrion can generate much more ATP via a more efficient process that requires oxygen, known as oxidative phosphorylation. The 2 NADH molecules from glycolysis generate about 5 molecules of ATP, and the whole process of glycolysis and oxidative phosphorylation combined produce around 32-34 molecules of ATP from your single molecule of glucose.
You can see that oxidative phosphorylation (in the mitochondria) produces far more ATP than glycolysis (outside the mitochondria).
How other fuels are converted into ATP energy

Your body can also generate ATP energy from other fuels.
Outside the mitochondria glycolysis can only generate ATP energy from glucose and in doing so also generates lactate.
We tend to think of lactate (or lactic acid) as a waste product that reduces muscular function when we exercise at a more intense level, but we now know that lactate has many benefits and also serves as a fuel source that can enter the mitochondria to generate ATP.
Fatty acids, amino acids and ketones can also be transported into the mitochondria as fuel to generate ATP energy by oxidative phosphorylation, and these fuels can only generate ATP energy in the mitochondria.
However your liver and kidneys can convert some of the amino acids and lactate into glucose to maintain blood sugar levels in between meals in a process known as gluconeogenesis.
Oxygen depletion shunts energy production to glycolysis
So now you understand that we need oxygen (despite its potential harmfulness) because without it we can’t generate ATP energy in the mitochondria and have to resort to generating ATP energy from glucose by the far less efficient process of glycolysis.
If oxygen is being used up to its maximum as in intense exercise when you get out of breath, oxidative phosphorylation reaches a saturation point and the less efficient but faster glycolysis takes over.
Although glycolysis is less efficient than oxidative phosphorylation, generating much less ATP energy from each molecule of glucose, it is nevertheless much faster in supplying the usable energy we need when our body is working at high intensity.
Since glycolysis can only generate ATP energy from glucose it depletes your stores of glycogen, the storage form of glucose. This glycogen store, primarily in your liver and muscles but also in your brain, is thus intended for short term emergencies, for ‘fight or flight’ situations.
Key differences between glycolysis and oxidative phosphorylation
| Glycolysis | Oxidative phosphorylation |
| Occurs outside of the mitochondria in the cytoplasm (the gelatinous liquid that fills a cell) | Occurs inside the mitochondria |
| Uses glucose as fuel | Uses glucose, amino acids, fatty acids, lactate and ketones as fuel |
| Low efficiency, generating a small amount of ATP | High efficiency, generating a large amount of ATP |
| Does not need oxygen | Depends on oxygen |
| Fast | Slow |
| Predominates at high intensity energy expenditure or when oxygen supply is short | Predominates at low/moderate intensity exercise or low/moderate energy expenditure |
| Generates lactate | Does not generate lactate |
20 causes of fatigue
Functional medicine for fatigue and CFS/ME must consider the root causes of fatigue. Many of these causes are interrelated and mutually dependent and I will discuss some of the interconnections below.
You might have just one main cause of fatigue, but my clients commonly have several or even many impactful causes.
1. Oxidative stress
When your mitochondria generate energy they also generate free radicals that can damage tissue. To protect the mitochondria from these free radicals you need antioxidants, some of which come from your diet and some of which are made inside your cells, glutathione being your main intracellular antioxidant.
If free radicals overwhelm your supply of antioxidants then you have oxidative stress and tissue damage is the result. The mitochondria which generate free radicals are particularly susceptible to free radical damage, and the resulting mitochondrial damage and dysfunction results in fatigue.
Boosting your intake of dietary antioxidants and supporting glutathione production can thus be helpful in reducing fatigue.
Oxidative stress also causes inflammation.
2. Inflammation
Chronic inflammation has been linked with fatigue and thus in many diseases which have been linked with inflammation we will also see fatigue. Examples of such diseases include autoimmune disease, cancer, diabetes and chronic fatigue syndrome.
The severity of fatigue in CFS/ME has been linked with the concentration of cytokines (inflammatory signalling molecules) in the blood and spinal fluid (6).
This fatigue can be understood as an intelligent response to conserve energy when dealing with an infection and to also encourage rest in order to reduce the transmission of pathogens (disease causing bacteria, viruses, fungi or parasites). The advantages of this response are similar to the evolutionary advantages of depressed mood also caused by inflammation.
There are several possible mechanisms by which inflammation can cause fatigue.
Inflammation is an activation of your immune system and the cells of your immune system need a rapid supply of energy from glucose, as is provided by glycolysis, which is faster but less efficient than oxidative phosphorylation. Chronic inflammation pushes the balance of ATP generation more towards glycolysis so that the total amount of ATP produced from each molecule of glucose is much reduced, although the ATP is produced more quickly, using up glycogen. Mitochondrial generation of ATP energy is reduced.
At the same time inflammation uses up more energy and thus decreases overall energy availability for other functions of the body yet increases your total energy expenditure by up to 10%.
Prolonged inflammation also causes insulin resistance, which means that your cells cannot take up glucose as readily and consequently cannot generate as much ATP energy from glucose.
Inflammation particularly affects energy availability in the nervous system. Neurons have high energy requirements and are rich in mitochondria. Thus when inflammation reduces mitochondrial function and there is lower glucose availability due to insulin resistance neurons become more dependent on the slower ATP production from lipids.
Inflammation also results in more oxidative stress, and as already discussed the mitochondria can easily be damaged by oxidative stress. Your immune cells release free radicals to attack invading pathogens as part of the inflammatory response and this is what causes the oxidative stress (7).
Cytokines are the signalling molecules of the inflammatory process. By communicating with the vagus nerve and by an effect on the blood brain barrier, cytokines in the blood stream can cause the elevation of cytokines in the brain and these impact the formation and function of neurotransmitters such as dopamine and serotonin. Dopamine is a neurotransmitter that supports your motivation so that poor dopamine function or low levels of dopamine could be a cause of mental fatigue (8).
In many conditions inflammation will also cause fatigue more indirectly through mechanisms specific to the condition.
For example in heart disease, be it coronary artery disease or heart failure, inflammation is a key driver, and yet much of the fatigue experienced in these conditions will be due to the compromised circulation of the blood and hence reduced delivery of nutrients and oxygen to the heart and other organs, where they are needed to generate ATP energy.
3. Stress

Short-term stress causes the release of a hormone (ACTH) from your pituitary gland which signals to your adrenal glands to release more of your stress hormone cortisol. Cortisol signals to many tissues in the body to provide you with more available resources (energy) to deal with the stressor and diverts resources away from less urgent needs.
For example, a cortisol elevation increases blood sugar, blood pressure, breathing rate and heart rate. The resulting increased availability of nutrients and oxygen is all intended to make usable energy more available where it is needed, such as in the brain and in the appropriate muscles for ‘fight or flight’.
Cortisol resistance
However your resources are limited and chronic stress with chronically elevated cortisol levels eventually leads to the cells of your body not responding to the cortisol signal, a state known as cortisol resistance.
At this point fatigue can set in, which can often be more pronounced on waking so that you are slow to get going in the morning and may be dependent on caffeine (9).
This is commonly referred to as burnout or adrenal fatigue.
Reduced signalling to the adrenal glands
However the term adrenal fatigue is not an accurate description of what is causing fatigue, since the adrenal glands which release cortisol do not get tired (10). With ongoing stress the signalling from the brain and pituitary gland to the adrenal glands eventually diminishes, and this is why the adrenal glands release less cortisol.
Burnout as an intelligent response
The combination of cortisol resistance and reduced cortisol release leads to what we call burnout. I think of this as an intelligent response to protect the body when resources have become too scarce for normal functioning.
But what exactly are these resources?
Glycogen depletion
Resources that are used up include glycogen, which is the storage form of glucose which your body calls upon in times of stress.
Glycogen stores can be replenished relatively quickly, provided stress does not continue to deplete them and provided you eat some carbohydrate foods.
Glycogen is intended for emergency use only, but when you are under chronic stress your body responds as if you are in a constant fight or flight emergency and depletes glycogen reserves to keep blood glucose levels high. The reason for the importance of glycogen or glucose availability during the fight or flight response (the stress response) will become clearer if you remember that glycolysis is the more rapid way of producing ATP energy and depends on one fuel only: glucose.

Micronutrient depletion due to stress
Micronutrients (vitamins and minerals) are also depleted by stress, and these include magnesium, zinc and vitamin B6 (11, 12). Vitamin C deficiency is also linked with stress (13) and supplementation may improve energy levels (14). A B-vitamin complex has been found to reduce the effects of stress (15).
Magnesium
Magnesium, which is also needed by the mitochondria to generate ATP energy, is rapidly lost in the urine when your body’s stress response is chronically activated. However. magnesium also plays a role in regulating the stress response and there is some evidence that magnesium deficiency will cause increased stress and anxiety (16), potentially resulting in a vicious cycle of stress causing magnesium loss and this causing more stress (17, 18) and more fatigue.
Zinc
Zinc also plays an important role in ATP energy production both in oxidative phosphorylation within the mitochondria and in glycolysis in the cytoplasm, the gel-like liquid that fills the cell outside of organelles like the mitochondria (19).
Zinc deficiency will also increase inflammation (20) and CFS/ME is associated with low serum zinc levels (21).
Low zinc levels have also been linked with an increased risk of depression (22), and depression has fatigue as one its symptoms.
Vitamin B6
Vitamin B6 supports blood sugar balance and methylation, but may also help to alleviate mental fatigue by another mechanism.
When you engage in cognitive work it has been shown that the tiredness that develops is associated with the buildup of the neurotransmitter glutamate in your prefrontal cortex. It is the build up of glutamate that is believed to cause the mental fatigue (23).
Vitamin B6 enables the activity of an enzyme that converts glutamate into GABA (24). Although GABA is known as a relaxing anti-anxiety neurotransmitter, it also supports learning and cognitive function in the prefrontal cortex, and especially tasks that involve holding information in your working memory (25).
Antioxidant depletion
Since cortisol pushes your metabolism to burn more fuel in your energy-generating mitochondria, it will increase the production of free radicals which can lead to oxidative stress (26, 27).
Thus your antioxidant reserve is another resource that is depleted by chronic stress.
If stress is causing your fatigue you can support your energy levels with both dietary antioxidants and by taking steps to increase your production of glutathione, your main endogenous (produced in the body) intracellular antioxidant (28).
Trauma in CFS/ME
Psychological trauma can drive an overactive stress response and can thus be a key driver in fatigue and CFS/ME.
Stress can cause fatigue indirectly
The body is a complex system and chronic stress affects many other systems of the body in a way that could result in fatigue, some of which will be discussed below.

4. Thyroid imbalances
Your GP may test you for TSH and T4 to determine if issues with your thyroid hormones could be causing your fatigue.
However this kind of testing is insufficient to rule out many potential issues with thyroid hormones and thyroid hormone function. TSH and T4 are not the active thyroid hormone that increases your metabolism, which is T3.
TSH (Thyroid Stimulating Hormone) is a hormone released by your pituitary gland to signal to the thyroid gland to produce and release more T4 thyroid hormone. T4 is then converted into the active thyroid hormone T3.
T3 and T4 reduce TSH signalling in a negative feedback loop which regulates thyroid hormone levels. Thus high levels of TSH or low levels of T4 could indicate low levels of thyroid hormone.
One shortcoming of just testing TSH and T4 is that T4 may not be getting adequately converted into T3 for a number of reasons.
Stress can have a negative impact on thyroid function in several ways, which includes reducing the conversion of T4 to T3.
5. Blood sugar dysregulation
High blood sugar, low blood sugar and big fluctuations in blood sugar can all cause fatigue (29).
When blood sugar goes up after a meal your pancreas releases insulin which signals to cells to take up the excess glucose. This prevents excess glucose from damaging tissue such as your artery walls and in this way insulin helps to prevent cardiovascular disease.
Glucose and fats are burned in the powerhouses of your cells: mitochondria. In the presence of excess glucose mitochondria do not burn the glucose effectively and produce an excess of free radicals which then damage the mitochondria themselves, further impeding energy production (30).
If blood sugar is chronically elevated from eating too much and too frequently, the cells reach a limit as to how much glucose they can take up and so they stop responding to normal and healthy levels of insulin. This is what we call insulin resistance and may result in the cells not being able to efficiently take up and use glucose for energy.
Since high blood sugar damages tissues it also activates the immune system to drive inflammation to respond to the damage (31), which may also increase demands on energy to some degree.
High blood sugar can also cause dehydration as your body tries to excrete the excess glucose in your urine and this can also contribute to fatigue, as can the loss of key micronutrients and the poor circulation that can result from chronically elevated blood sugar.
On the other hand those gym and diet warriors who are particularly zealous in their battle against high blood glucose can go too far. Without sufficient carbohydrate to match the requirements of an intense exercise program glycogen is depleted, as can also be the case by simply restricting carbohydrate foods too much.
Glycogen depletion can result in low blood glucose levels which in itself can cause fatigue and sleepiness. The sleepiness can be immediate but if hypoglycaemia occurs in the night you may feel more fatigue the following day. Moreover the resulting low insulin levels are one of the factors that cause a poor conversion of T4 to T3 and hence more fatigue as metabolism slows down.
Since cortisol raises blood sugar, chronic stress can drive insulin resistance and this is another way in which stress can cause fatigue (32).
Blood sugar can be effectively balanced with dietary and lifestyle changes alone.
6. Mitochondrial dysfunction
Since mitochondria produce most of your energy, any damage to your mitochondria or any dysfunction of your mitochondria will cause fatigue. The generation of ATP for usable energy switches from the more efficient oxidative phosphorylation inside the mitochondria to glycolysis outside the mitochondria, resulting in much lower ATP production from each molecule of glucose. Fatty acids and amino acids that now cannot be used to generate ATP in the mitochondria need to be converted into glucose before they can be used in glycolysis to make ATP outside of the mitochondria.
The far-reaching effects of mitochondrial dysfunction in CFS/ME
Mitochondrial dysfunction is a hallmark of CFS/ME and effective treatment of CFS/ME must improve mitochondrial function (33).
Earlier I discussed how fluoroquinolone antibiotics can target mitochondria and can cause severe symptoms of dysautonomia, the name implying a failure of the autonomic nervous system to regulate blood pressure, heart rate and body temperature. This may be because neurons are rich in mitochondria as they need a lot of energy to transmit nervous impulses.
However it has also been suggested that the same symptoms of feeling faint, low blood pressure, dizziness, and elevated heart rate that also occur in CFS/ME could be due to poor blood circulation as a result of the failure of mitochondria in heart muscle. The heart has a very high density of mitochondria as you might expect given its huge 24/7 workload.
However you may be surprised to learn that the retina is the tissue in the body that is the most dense in mitochondria (34), since it takes a lot of energy for photoreceptors to generate nerve impulses from photons of light. This may be why CFS/ME sufferers tend to have issues with their eyes, such as light sensitivity.
Causes of mitochondrial damage and dysfunction
We have already seen how blood sugar elevations and oxidative stress can damage mitochondria, but there are many other factors that can cause mitochondrial dysfunction, some of which are discussed below.
7. Micronutrient insufficiencies or imbalances

I have already discussed the role of magnesium, zinc and vitamin B6 in energy production and how vitamin C is also linked with energy levels, as these micronutrients are depleted by chronic stress.
Micronutrients (vitamins and minerals) act as essential cofactors that enable enzymes to perform their functions, which include many steps in the process of ATP energy generation.
Mitochondria depend on a sufficient supply of certain micronutrients to produce energy, so that a deficiency or insufficiency is one cause of mitochondrial dysfunction.
B-vitamins, for example, play essential roles at various steps in the generation of ATP energy in the mitochondria (35).
The oral contraceptive pill depletes key micronutrients such as some of the B-vitamins that can play a role in ATP energy production (36, 37).
Statins are known to deplete CoQ10 which is a key nutrient and antioxidant required by mitochondria. This is the likely reason why statins cause fatigue in some individuals (38).
An excess of a particular micronutrient can also be a cause of fatigue.
Copper is vital for effective mitochondrial function but in excess will damage the proteins and lipids of mitochondria, cause oxidative stress and deplete the antioxidants that protect the mitochondria (39).
Iron deficiency anaemia is a common cause of fatigue, since iron is a vital component of haemoglobin, which binds to oxygen in red blood cells and thus enables the transport of oxygen to the tissues where it is needed to produce ATP energy in the mitochondria.
On the other hand an excess of iron will drive oxidative stress that will damage mitochondria (40).
8. Insomnia
Be it difficulty falling asleep or staying asleep, insomnia causes fatigue (41).
This should come as no surprise as we understand sleep to be a time to rest and recover so that we can be functional during the day.
Aside from the missed opportunity to recuperate and repair, sleep loss also drives inflammation, and inflammation drives further insomnia in a vicious cycle (42).
Inflammatory conditions often cause pain. Pain both causes and is caused by insomnia in a further self-perpetuating cycle that will increase fatigue (43).
Stress can play a big role in insomnia (44).
Blood sugar dysregulation can disrupt sleep and sleep disruption can cause insulin resistance and blood sugar dysregulation in a bidirectional relationship (45).

9. Obesity and overnutrition
Overnutrition is the eating of more nutrients than you need, but the most relevant aspect of overnutrition for fatigue is the overeating of foods rich in fat, protein and carbohydrate that can be used to generate ATP energy, leading energy excess, weight gain and obesity.
Overnutrition causes mitochondrial dysfunction, oxidative stress, inflammation and insulin resistance
This kind of overnutrition leads to an excess of ATP being generated in the mitochondria and correspondingly a large number of free radicals are produced by the mitochondria. The resulting oxidative stress damages mitochondria so that fat burning is then reduced, leading to weight gain and obesity (46). The decreased capacity of the mitochondria to generate ATP energy from fatty acids and glucose causes fatigue, and this can often manifest as rapidly getting tired on physical exertion (47).
With oxidative stress comes inflammation. Inflammation, oxidative stress and mitochondrial dysfunction all drive each other in a vicious cycle (48) and cause insulin resistance (49, 50) and thus even more fatigue.
Overnutrition can cause mitochondrial dysfunction in the hypothalamus
These effects can also affect the brain and central nervous system, as well as the blood brain barrier (51).
In the brain the hypothalamus senses and helps to regulate blood glucose, communicating with the pancreas which releases the hormones insulin and glucagon to regulate blood sugar. This sensing of glucose levels depends on mitochondria in the hypothalamus, which can be affected by the oxidative stress from an excess of fat tissue (52), thus strengthening the vicious cycle of oxidative stress, inflammation, mitochondrial dysfunction, insulin resistance and fatigue.
Mitochondrial dysfunction in fat cells may reduce adiponectin to cause more inflammation
Mitochondria in white fat cells are responsible for making the hormone adiponectin, which increases insulin sensitivity and reduces inflammation and the build-up of arterial plaque that causes heart disease. It has been proposed that dysfunction of mitochondria in the white fat cells and a corresponding decrease in adiponectin could be a major cause of inflammation in fat tissue (53).
Obesity and insomnia
Obesity can also increase the risk of insomnia and insomnia in turn increases the risk of obesity in another vicious cycle (54).
Obesity reduces testosterone and increases oestrogen in men
Fat tissue contains aromatase, an enzyme that converts testosterone to oestrogen. An excess of fat tissue can therefore be a cause of low testosterone and high oestrogen in men.
Testosterone deficiency in men can also cause more weight gain as well as insulin resistance (55), resulting in another vicious circle.
10. Oestrogen and testosterone imbalances

Both oestrogen and testosterone enhance oxidative phosphorylation in the mitochondria.
The effects of low testosterone in men and in women
In men low testosterone can be a cause of insulin resistance, though in women high testosterone is linked with insulin resistance.
One hypothesis for why high testosterone in women can cause insulin resistance is that because oestrogen is higher in women it may act synergistically with the elevated testosterone to increase ATP generation in the mitochondria to such an extent that we get the same effect as we do in the way that overnutrition causes insulin resistance: an overproduction of free radicals damaging the mitochondria (56).
Fatigue is one of the symptoms of low testosterone in both men and women. Testosterone reduces fatigue by enhancing mitochondrial function, regulating metabolism and improving the uptake of glucose by your muscles (57). Testosterone also helps to reduce inflammation (58).
The relationship between testosterone deficiency and insulin resistance appears to work both ways, potentially forming a self-perpetuating cycle (59).
Why the promotion of testosterone replacement therapy (TRT) is dangerously irresponsible
You may have heard that testosterone declines with age, but there is increasing evidence that this does not occur in men who maintain good health and is a result not of ageing per se but of the comorbidities that tend to increase with age as a result of dietary and lifestyle factors, which would include insulin resistance and obesity (60).
There has been a substantial decline in testosterone levels and sperm counts over the 20th century, in parallel with a steep rise in the rates of obesity, diabetes and metabolic syndrome. This suggests that rapidly changing dietary, lifestyle and environmental factors are likely to be at play.
The effects of the modern diet on metabolic health and fertility may be passed down and multiplied from each generation to to the next since diet and lifestyle affect the switches or markers that cause genes to be silenced or to be expressed or active. These markers are then inherited and further influenced by diet and lifestyle in the next generation. The study of these markers and their behaviour is known as epigenetics (61).
Working on reducing the root causes of testosterone deficiency would be the more naturopathic or functional medicine approach to reducing fatigue and other symptoms of low testosterone, rather than relying on the heavily marketed testosterone replacement therapy (TRT) with all of the inherent risks and potential side effects that come with it. Resorting to TRT avoids dealing with underlying causes that could then potentially reduce your life by years and your healthspan by decades, because low testosterone is not the only effect these underlying causes have.
Some studies link TRT with an increased risk of heart disease, stroke, prostate enlargement, prostate cancer, infertility, acne, fluid retention, sleep apnea, gynecomastia (breast enlargement) and liver toxicity (62). These side effects tend to be played down on TRT clinic websites.
If you are converting the exogenous testosterone (exogenous meaning produced outside the body) into oestrogen due to being overweight or obese rather than losing weight, you may need to inhibit this conversion by also taking aromatase inhibitor drugs which have their own additional set of potential side effects.
Causes of low testosterone
I have already mentioned a few causes of fatigue that can also cause low testosterone in men: stress, blood sugar dysregulation, being overweight or obese, micronutrient deficiencies, hypothyroidism and oxidative stress, which can damage the testosterone-producing Leydig cells in the testes (63).
I will mention a few more causes of both testosterone deficiency and fatigue below.
Oestrogen in menopause and perimenopause
Women in perimenopause or menopause may experience fatigue due to oestrogen fluctuations or low oestrogen levels, which can also impact sleep and drive increased levels of stress.
11. Environmental toxins (toxicants)

Environmental toxins (or toxicants) are another cause of low testosterone in men and hence fatigue. Pesticides, heavy metals such as lead and cadmium and particulate matter in air pollution can all cause oxidative stress that can damage Leydig cells in the testes and also cause low testosterone by multiple other mechanisms. Endocrine disrupting chemicals found in plastics and many other products mimic oestrogen, can interfere with testosterone receptors and also reduce testosterone by other mechanisms (64). Many of these toxicants are also obesogens, meaning they cause weight (fat not muscle) gain.
Another way in which toxins can cause fatigue is by damaging mitochondria or causing dysfunction of mitochondria. I have already discussed how certain antibiotics can damage mitochondria, but mitochondria are also very sensitive to many other drugs and many environmental toxicants.
Toxins cause oxidative stress which can cause damage to the mitochondria and they can also directly damage mitochondrial DNA, enzymes and other proteins in the mitochondria.
Many toxins are fat soluble and thus accumulate in the fatty mitochondrial membranes, such as polycyclic aromatic hydrocarbons (PAHs) which can be present in grilled meat and fish.
Toxins that damage mitochondria and cause mitochondrial dysfunction include polycyclic aromatic hydrocarbons (PAHs), copper, arsenic, mercury, cadmium, lead, PFAS, carbon monoxide, methanol, cyanide, bacterial endotoxins, particulate matter (from air pollution), cigarette smoke, acrylamide and some pesticides and herbicides such as rotenone and paraquat (65).
Some toxicants can also dysregulate blood sugar and cause insulin resistance to further drive fatigue (66).
Toxins and micronutrients
Toxins can also deplete micronutrients to cause more fatigue.
For example, mercury and some food colourings have been shown to deplete zinc (67).
Your body has natural biochemical pathways that can detoxify many toxins. Since these detoxification pathways are dependent on specific micronutrients, an increased toxic burden due to poor detoxification is another way in which micronutrient deficiencies can cause fatigue.
Thus we have a bidirectional relationship between toxic burden and micronutrient status, and this could function as another self-perpetuating cycle.
12. Methylation issues
Methylation is a biochemical process that is vital for numerous essential processes in your body, including energy production in the mitochondria (68), supporting immune function to fight off infections that when out of control will cause more fatigue and for the formation of key molecules involved in the process of generating ATP such as carnitine and Coenzyme Q10. Methylation also supports neurotransmitter production.
Methylation is dependent on B-vitamins and certain other micronutrients, and supplementing these can help sufferers of CFS/ME (69).
Besides suboptimal levels of these nutrients and certain genetic variants, poor methylation can also have many other causes which may need to be investigated if lab testing indicates an issue with methylation.
For example certain toxins, such as methylmercury (the form of mercury found in fish), alcohol and acetaldehyde, can inhibit key enzymes involved in methylation (70).
13. Gut dysbiosis and leaky gut

Gut dysbiosis effect on nutrients, toxins and immune system
Gut dysbiosis can result in toxins being released from bacteria and fungi that can cause fatigue. It can also cause nutrient malabsorption and inflammation and weakens the immune system against infections, all of which cause further fatigue.
Endotoxins
Endotoxins from bacteria can enter the blood stream, and more so when there is ‘leaky gut’. Endotoxins are highly inflammatory and thus cause fatigue and potentially chronic fatigue, brain fog and many other symptoms and conditions, including severe mental illness (71, 72, 73).
Overgrowth of candida albicans and other fungal species
A very common cause of fatigue I see in my clinical practice is due to overgrowing fungal species, such as candida albicans.
Many sufferers of CFS/ME have a prior history of IBS and of the use antibiotics in early childhood. By diminishing counts of lactobacilli bacteria, which help to keep candida under control, antibiotics in early life may have set the stage for fungal overgrowth. This could be the cause of the IBS and as it progresses throughout life could be the eventual cause of CFS/ME (74).
Fatigue from fungal overgrowth could be due to leaky gut, inflammation and nutrient depletion, but candida and other species release a whole array of very potent toxins, which clinical experience leads me believe to be the most significant driver of fungal-related fatigue.
Acetaldehyde, which also causes hangovers, is one particularly potent fungal toxin produced in significant quantities by most candida species and plays a role in the formation of protective biofilm that makes candida overgrowth so difficult to eradicate (75). Acetaldehyde causes fatigue by increasing inflammation, causing hypoglycaemia (low blood sugar) and disrupting sleep. Acetaldehyde in the gut results in increased levels of bacteria of the type that produce endotoxins and it causes leaky gut that enables more of these endotoxins to enter the bloodstream to drive inflammation and fatigue, as we know from research on long term drinkers (76).
Leaky gut could be one reason why CFS/ME patients crash after physical exertion
In CFS/ME sufferers attempting to exercise is likely to cause a crash. This effect may be in part due to the gut becoming more permeable (‘leaky’) when exercising, which can allow bacteria to enter the bloodstream and cause inflammation (77).
Gut dysbiosis can disrupt sleep
Gut dysbiosis can also cause fatigue by disrupting sleep. This is in part because the microbiome regulates compounds that play a role in sleep and wakefulness such as the neurotransmitter serotonin and the stress hormone cortisol (78). Certain bacterial species in your gut produce short-chain fatty acids such as the anti-inflammatory butyrate, which also induces sleep and can be low when there is gut dysbiosis (79). CFS/ME patients have been found to have low levels of key butyrate-producing bacteria and these low levels have been linked with fatigue in CFS/ME (80).
Gut dysbiosis can disrupt hormones
Your gut microbiome can also affect hormones such as testosterone, oestrogen and thyroid, and this is another reason why reducing gut dysbiosis could improve your energy levels (81, 82, 83).
Stress can also cause fatigue by impacting the gut
There are many ways in which stress affects the gut and can cause gut dysbiosis and this is yet another way in which chronic stress can cause fatigue.
14. Infections
Infections tend to cause fatigue which can continue for some time after the infection.
This is believed to be a way that the body conserves energy.
Neuroinflammation (inflammation of the nervous system) may be behind this fatigue and there is evidence of neuroinflammation in CFS/ME (84).
According to a large observational study infections of many kinds are associated with an increased risk of CFS/ME (85) and infections by viruses such as the Epstein-Barr virus and herpes viruses are often reported as triggers of CFS/ME. It has been proposed that some kind of immune system dysregulation is at play in CFS/ME (86).
Candida albicans intestinal overgrowth depresses the immune system in such a way that could cause latent viral infections get reactivated and thus cause CFS/ME (87).
Stress can be another cause of poor immune function (88).
15. Ultra-processed foods
Ultra-processed foods are highly inflammatory and have been linked with a higher risk of type 2 diabetes (89) and drive weight gain and obesity (90), all of which cause fatigue.
Ultra-processed foods affect your brain in a way that makes them highly addictive. This in itself will cause overnutrition and hence fatigue.
The lack of fibre in such products causes gut dysbiosis (91) and many emulsifiers and potentially other additives will cause further gastrointestinal inflammation (92).
Ultra-processed foods are also low in many micronutrients, some of which are crucial for the generation of ATP energy (93).

16. Food intolerance
Food intolerances such as intolerance to gluten or lactose can also cause fatigue, amongst many other symptoms (94).
17. The wrong amount of exercise
Exercise for physical strength and energy
Exercise can improve energy levels and feelings of vitality (95). Physical inactivity reduces muscle mass and strength and your muscles become less efficient and tire more easily. Exercise can increase your muscle mass, strength and efficiency to reverse this effect (96).
How exercise benefits your mitochondria
One way in which your body adapts to exercise that benefits your energy levels is by increasing the number of and the efficiency of your mitochondria, not just in your muscles but in your brain and likely in other tissues as well (97).
Exercise for blood glucose regulation
Exercise also increases glucose uptake into muscles by up to 100-fold, thus helping to regulate blood glucose. How much more glucose is taken up compared to when being at rest depends on the intensity and duration of the workout, and the effect lasts up to 48 hours (98, 99).
Exercise to turn on health-promoting genes
Exercise is just one example of a stressor that can turn on genes that promote health with far-reaching consequences which will also improve overall energy levels by many means, such as reducing inflammation and improving detoxification.

Exercise that increases testosterone in men
High intensity exercise such as High-Intensity Interval Training (100) and resistance training (101) also increases testosterone in men which can support energy levels.
Overtraining
Overtraining, however, will reduce testosterone in men (102) and will harm mitochondria (103).
Earlier I discussed how chronic stress can cause fatigue. This stress can include not just psychological stress by also physical stress from doing too much exercise.
If you have CFS/ME, even making your dinner, washing the dishes or getting out of bed could constitute over training.
18. Dehydration
Dehydration can cause some degree of fatigue, as well as poor cognitive function and mood (104).
19. Alcohol
Alcohol will cause fatigue by disrupting sleep (105) and blood sugar regulation (106), as well as causing a loss of micronutrients vital to ATP energy production, such as B-vitamins (107), magnesium (108) and zinc (109).
Chronic alcohol use could also be causing fatigue in men by increasing oestrogen and reducing testosterone levels (110) and by causing dehydration, since alcohol is a diuretic.
20. Excess caffeine

Caffeine tolerance and wearing off effects on energy
If you develop a tolerance to caffeine you may feel tired before your morning cup.
You may also experience the tiredness you masked with caffeine when the caffeine wears off, and this tiredness may be amplified.
Caffeine can cause dehydration
Caffeine is a diuretic, which means that it causes you to urinate more and this can cause dehydration and hence fatigue.
Caffeine increases blood sugar that can make you tired
Although one of coffee’s many health benefits is sometimes said to be due to benefiting blood sugar in the long term, that effect appears to be due to the beneficial polyphenols it contains, and especially chlorogenic acid.
Caffeine itself appears to reduce insulin sensitivity in the short term, meaning that your insulin is not so effective in getting cells to take up glucose from the blood. Consequently glucose may be elevated after your cup of coffee (111, 112).
This could potentially make you more tired instead of stimulated when you drink coffee.
You might be surprised to learn that caffeine has anti-fungal properties and can even help break down the protective biofilm that fungal species like candida albicans can hide behind for self-protection (113).
However in my clinical practice I see time and time again that caffeine exacerbates fungal overgrowth, and in my opinion this is likely to be because of the effect of caffeine-driven blood sugar fluctuations on candida overgrowth.
How even morning coffee could disrupt your sleep to cause fatigue

Then of course caffeine can cause fatigue by reducing the quality and duration of your sleep if you take it too close to bedtime (114).
But what exactly do we mean by ‘too close to bedtime’?
The half-life of caffeine in your blood ranges from around 2 to 12 hours (115). How fast you metabolise caffeine depends largely on genetics but there are also some ways in which you can speed up your metabolism of caffeine.
Furthermore, the caffeine is broken down into three metabolites which are also stimulants and have their own half-lives, though shorter than that of caffeine.
If you are a slow metaboliser of caffeine, therefore, it could take almost 12 hours for just half of the caffeine to leave your bloodstream and at 24 hours caffeine could be at around a quarter of its peak. This means that even if you have your coffee early at 7am a quarter of the caffeine will still be in your blood stream at 7am the following day, and stimulating caffeine metabolites will also still be having an effect all through the night.
Functional medicine for fatigue & CFS/ME at London, Devon and online clinics
Functional medicine for fatigue and CFS/ME encompasses a multi-pronged approach. Since there are so many potential causes of fatigue – and often several causes are at play simultaneously – a breadth and depth of knowledge is called for. Specialising exclusively in any one particular area, be it methylation, endocrine health, gut health or any other area, will mean that most causes of fatigue and CFS/ME will be missed. Hence I maintain a breadth and depth of knowledge that enables me to provide effective support for fatigue and CFS/ME clients., making use of my skills as both a nutritionist and a lifestyle medicine practitioner.
It is always the aim of functional medicine to treat each person as an individual and to find the specific root causes of each individual’s symptoms. To this end I use detailed health questionnaires, diet diaries, functional lab tests and sometimes genetic testing and form a more complete picture in conversation with you during each consultation.
Functional lab testing for fatigue & CFS/ME
Functional lab testing helps to tailor my dietary and lifestyle recommendations towards your individual needs to optimise your energy levels. I use the information I have already gathered about you to recommend the most appropriate testing.
Functional lab tests for fatigue and CFS/ME may include:
- Stress hormone and sex hormone testing, such as the DUTCH test or the HuMap test
- Thyroid hormone testing
- Stool testing
- Micronutrient testing
- Testing for environmental toxins including
- mycotoxins from mould exposure
- heavy metals
- other industrial pollutants
- Methylation testing
- Virus testing
- Food sensitivity testing
Find out more about working with me
Find out more about how I apply the principles of functional medicine, nutritional therapy and naturopathy at my clinics in London, Devon and online.
Book a free no-obligation 20-minute telephone appointment using the box to the right near the top of the page to ask any further questions you may have about working with me to optimise your energy levels and to book an initial consultation.





